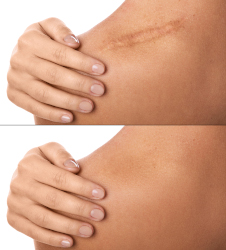
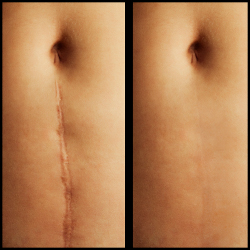
Scar Revision
Minimize a Scar
Scar revision is a plastic surgery procedure performed to improve the condition and/or appearance of a scar anywhere on your body, so that it is more consistent with your surrounding skin tone and texture.
Scars are visible signs that remain after a wound has healed. They are unavoidable results of injury or surgery, and their development can be unpredictable. Poor healing may contribute to scars that are obvious, unsightly or disfiguring. Even a wound that heals well can result in a scar that affects your appearance. Scars may be raised or recessed, different in colour or texture from surrounding healthy tissue or particularly noticeable due to their size, shape or location. The different types of scars include:
-Discoloration, surface irregularities and other more subtle scars can be cosmetically improved by surgery or other treatments recommended by your plastic surgeon. These types of scars do not impair function or cause physical discomfort and include acne scars as well as scars resulting from minor injury and prior surgical incisions.
– Hypertropic scars are thick clusters of scar tissue that develop directly at a wound site. They are often raised, red and/or uncomfortable, and they may become wider over time. They can be hyperpigmented (darker in colour) or hypopigmented (lighter in colour).
– Keloids are larger than hypertropic scars. They can be painful or itchy, and may also pucker. They extend beyond the edges of an original wound or incision. Keloids can occur anywhere on your body, but they develop more commonly where there is little underlying fatty tissue, such as on the face, neck, ears, chest or shoulders.
– Contractures are scars that restrict movement due to skin and underlying tissue that pull together during healing. They can occur when there is a large amount of tissue loss, such as after a burn. Contractures also can form where a wound crosses a joint, restricting movement of the fingers, elbows, knees or neck.
The type of scar you have will determine the appropriate techniques your plastic surgeon will use to improve your scar. Your treatment options may vary based on the type and degree of scarring and can include:
- Simple topical treatments
- Minimally invasive procedures
- Surgical revision with advanced techniques in wound closure
Although scar revision can provide a more pleasing aesthetic result or improve a scar that has healed poorly, a scar cannot be completely erased.
Before the operation
Prior to scar revision surgery, you may be asked to:
- Get lab testing and/or a medical evaluation
- Take certain medications or adjust your current medications
- Stop smoking well in advance of surgery
- Avoid taking aspirin and certain anti-inflammatory drugs and herbal supplements as they can increase bleeding
Special instructions you receive will cover:
- What to do on the day of surgery
- The use of anaesthesia during your procedure
- Post-operative care and follow-up
Hospital stay and type of anesthesia
Type of anesthesia: Medications are administered for your comfort during the surgical procedures. The choices include local anaesthesia, intravenous sedation and general anaesthesia. Your doctor will recommend the best choice for you.
Hospital stay: The surgery is usually done in the “day care” department; this means that you can leave the hospital the same day of the surgery, after a few hours of medical supervision.
The procedure
Step1
The degree of improvement that can be achieved with scar revision will depend on the severity of your scarring, the type, size and location of the scar. In some cases, a single technique may provide significant improvement. However, your plastic surgeon may recommend a combination of scar revision techniques to achieve the best results.
Topical treatments, such as gels, tapes or external compression, can help in wound closure and healing, or to reduce the ability of skin to produce irregular pigment. These products may be used to treat existing surface scars and discoloration, and to aid in healing of scar revision procedures.
Injectable treatments are often used to fill depressed or concave scars. Depending on the injectable substance used and your particular scar conditions, results may last from three months to several years. Therapy must be repeated to maintain results. One form of injection therapy uses steroidal-based compounds to reduce collagen formation and can alter the appearance, size and texture of raised scar tissue.
Surface treatments are most often used for aesthetic improvement of scars. These methods can soften surface irregularities and reduce uneven pigmentation. Surface treatments are a controlled means of either mechanically removing the top layers of skin or changing the nature of tissue. These treatment options include:
- Dermabrasion is a mechanical polishing of the skin.
- Laser or light therapy causes changes to the surface of the skin that allow new, healthy skin to form at the scar site.
- Chemical peel solutions penetrate the skin’s surface to soften irregularities in texture and colour.
- Skin bleaching agents are medications applied topically to lighten the skin.
Step 2 – Sometimes for deeper scars an incision is needed to surgically remove the old scar.
Step 3– Closing the incisions:
Some scars require layered closure. Layered closure is often used where excision extends to tissue below the skin surface or in areas with a high degree of movement. The first step, or layer, requires sub-dermal closure (below the skin surface) with absorbable or non-removable sutures. Layers of closure continue to build, concluding with closure of the remaining surface wound.
Advanced techniques in scar revision include complex flap closure to reposition a scar so that it is less conspicuous, or improve flexibility where contracture has restricted mobility.
Pharmaceutical tissue substitutes may be used if ample healthy tissue is not present for closure of a scar excision. This is more likely with revision of severe burn scars.
Tissue expansion can be a substitute for skin grafts. In this procedure, an inflatable balloon called a tissue expander is placed under the skin near the scar site. Over time, the balloon is slowly filled with sterile solution to expand the area of healthy skin. Once the skin has been stretched sufficiently, the expander and the scar is removed and the stretched skin is moved to replace the scar tissue. This process can involve multiple surgical stages or procedures in order to achieve the final results.
After the operation
Progress and healing:
The initial healing phase of a surgical scar revision may include localized swelling, discoloration or discomfort and may take 1 to 2 weeks. Healing will continue for several weeks and as the new scar heals it will slowly refine and fade. With dermabrasion, chemical peel or laser resurfacing, you will experience similar conditions at the treated area, in addition to overall sensitivity.
When you go home:
If you experience shortness of breath, chest pains, or unusual heart beats, seek medical attention immediately. Should any of these complications occur, you may require hospitalization and additional treatment.
Be careful: Following your surgeon’s instructions is key to the success of your surgery. It is important that the surgical incisions are not subjected to excessive force, abrasion, or motion during the time of healing. Your doctor will give you specific instructions on how to care for yourself.
Follow all postoperative instructions carefully, including cleansing and at-home treatment regimens, and avoid sun exposure. Your cooperation will influence the outcome of your surgery.
Picture Gallery
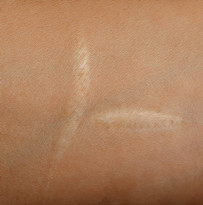
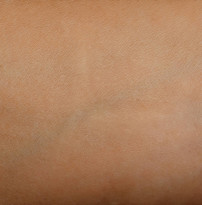
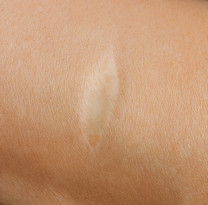
The result
The final results of your scar revision surgery will be long-lasting, however it may take several months for your final results to become apparent and in some cases it may take a year for the new scar to fully heal and fade.
Imperfect results
Although good results are expected, there is no guarantee, in some situations, it may not be possible to achieve optimal results with a single surgical procedure and another surgery may be necessary
Possible complications
The decision to have scar revision surgery is extremely personal and you’ll have to decide if the benefits will achieve your goals and if the risks and potential complications are acceptable. Your plastic surgeon and/or staff will explain in detail the risks associated with surgery.
You will be asked to sign consent forms to ensure that you fully understand the procedure you will undergo, the alternatives and the most likely risks and potential complications.
Some of the risks include:
- Bleeding (hematoma)
- Infection
- Delayed healing
- Anesthesia risks
- Change in skin sensation
- Damage to deeper structures including nerves, blood vessels, muscles and lungs can occur and may be temporary or permanent
- Allergies to tape, suture materials and glues, blood products, topical preparations or injected agents
- Skin contour irregularities
- Skin discoloration and swelling
- Skin sensitivity
- Deep vein thrombosis, cardiac and pulmonary complications
- Pain, which may persist
- Possibility of revisional surgery or staged procedures
Be sure to ask questions: It’s very important to ask your plastic surgeon questions about your procedure. It’s natural to feel some anxiety, whether it’s excitement for your anticipated new look or a bit of preoperative stress. Don’t be shy about discussing these feelings with your plastic surgeon.
My Way …. “Metron Ariston”
In case of depressed or concave scars, I opt for using dermal fillers and/or autologous fat transfer to fill in the defect.
Autologous fat transfer is also the treatment of choice for filling post-burn and post-traumatic scars. There are numerous advantages in fat transplant, as fat tissue is an important source of adult mesenchymal stem cells, allowing the regeneration of tissues in the recipient area.
For deeper Contracture scars demanding surgical removal, I use the Z-plasty or W-plasty techniques to alter the direction of the scars, and conceal them within natural folds.
This webpage aims to provide some information about the subject. Individual patient circumstances may differ, which might alter both the advice and course of therapy given to you by your doctor.
Source:
American Society of Plastic Surgeons, British Association of Plastic, Reconstructive and Aesthetic Surgeons, French Society of Plastic, Reconstructive and Aesthetic Surgery
